We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
.jpg)
-1.png?width=300&name=My%20Post%20(19)-1.png) Bleeding during pregnancy is scary, particularly when you have been trying to get pregnant for a long time with the help of a fertility specialist. In this post, I’m going to look at different reasons why bleeding happens during early pregnancy—including reasons that DON’T involve miscarriage.
Bleeding during pregnancy is scary, particularly when you have been trying to get pregnant for a long time with the help of a fertility specialist. In this post, I’m going to look at different reasons why bleeding happens during early pregnancy—including reasons that DON’T involve miscarriage.
Please note that if you’re very worried about bleeding, especially heavy bleeding accompanied by pain, cramps, or clots, you should call your physician first and follow his or her advice.
Our first response when bleeding occurs in this very much-desired pregnancy is “Oh no! I must be miscarrying!” “What did I do wrong?” “Why is this happening to me?” Well, I am going to tell you to STOP this negative talk to yourself. It is unlikely that you did anything wrong. Yes, it is certainly scary. Yes, it could be the first sign of a miscarriage. But we also see bleeding in many pregnancies that continue to term. In fact, it is very common to have some bleeding during pregnancy. About 27% of all pregnancies have some bleeding without an immediate miscarriage.
So that is a lot of pregnant women who experience bleeding and not all result in miscarriage. Most do not miscarry. About 15% of all pregnancies will miscarry. This percentage does go up as women age—to about 35% in women in their early 40’s.
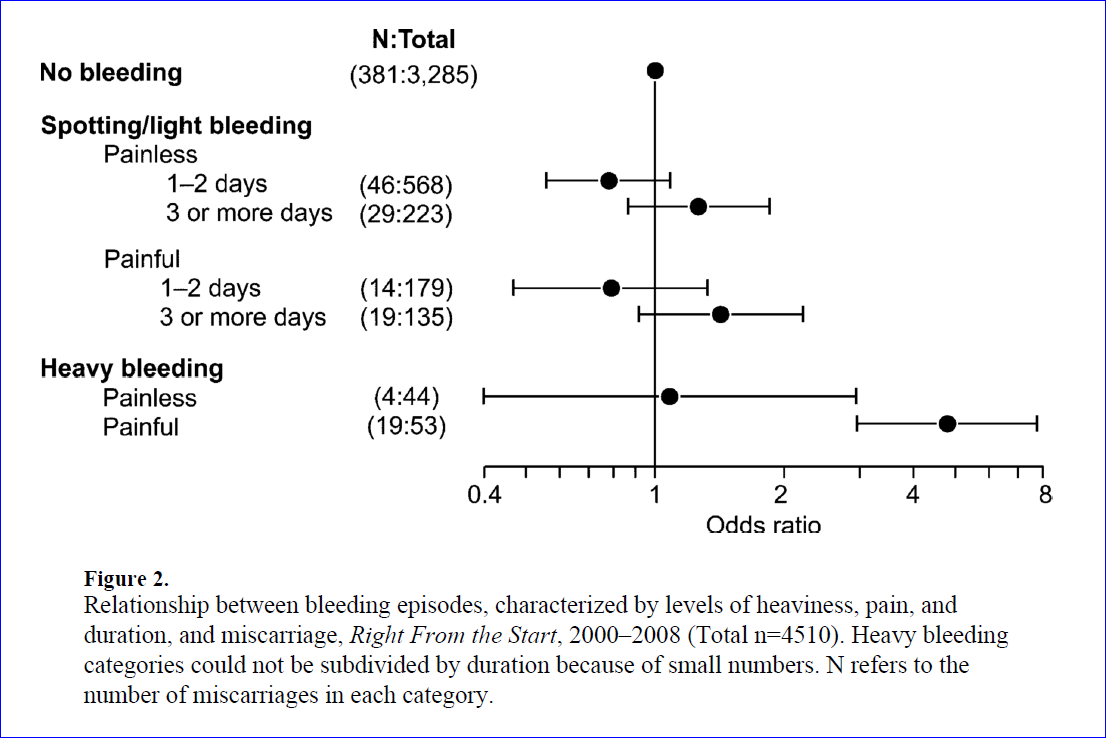
So why do so many pregnant women bleed? See the chart above. This figure shows that bleeding associated with cramping came at a high risk for miscarriage. Other pregnancies with reported bleeding but no pain or cramping in this figure did not result in miscarriage any more often than pregnancies with no reported bleeding.
There may be many reasons why a pregnant woman may bleed. Women notice bleeding on bath tissue and sometimes it is hard to tell where this bleeding is coming from. One place that bleeding on bath tissue may come from is the rectum or anus, particularly if there are hemorrhoids. In these cases, bleeding may be noticed after a bowel movement.
Bleeding from a hemorrhoid may be light or can be heavier, depending on the inflammation of the hemorrhoid. This type of bleeding may resolve on its own, after some pressure is applied, or it may need some treatment to resolve (a stool softener, Preparation H, steroid cream, or other treatment).
Bleeding may also come from an infection in the vagina or the bladder. If the patient has a vaginal infection (very common ones include yeast infections or bacterial vaginitis—“BV”) or vaginal/vulvar warts, these problems may result in bleeding during pregnancy. Treatment will resolve these issues. A bad bladder infection or inflammation of the bladder (cystitis) may result in bloody urine that can be confused with pregnancy-related bleeding.
However, if there is an infection, the bleeding may be accompanied by burning on urination. This infection or cystitis will need to be treated with antibiotics that are safe to use during pregnancy (your physician and pharmacist will be able to help prescribe appropriate medication). Once treated this bleeding should stop.
Bleeding may occur from the cervix which is the portion of the uterus where it opens into the vagina. Bleeding may occur on tissue or may discolor the water in the toilet bowl when urinating and still be coming from the cervical bleeding. This type of bleeding may be noticed after a transvaginal ultrasound, after a pap smear, or after intercourse because the cervix may be bumped during these activities and the cervix is more sensitive during pregnancy.
The reason that the cervix is more sensitive is that the cervix has cells that are normally located in the cervical canal where they are not able to be bumped. During pregnancy these cervical canal cells move to the outer portion of the cervix due to raised estrogen levels. This displaced layer of cervical cells is thinner than normal.
So when women walk, have intercourse, a pap smear, or a transvaginal ultrasound, the cervix may be “bumped” where these thinner layer cells are present and result in bleeding. This type of bleeding usually resolves on its own unless the patient is taking a blood thinner or an aspirin product which interfere with the blood being able to clot well on its own.
Sometimes there is bleeding coming from a portion of the pregnancy when a small area of the gestational sac pulls away from the uterus with some bleeding behind it. This bleeding may track down to the cervix and come out. This area may be seen on ultrasound and it is called a subchorionic bleed---which I will discuss in another blog. These too can be fairly prevalent and most resolve without a problem during pregnancy.
Bleeding may occur and resolve without us finding a reason for the bleeding. In these situations, we often watch the pregnancy a little closer with more frequent ultrasounds to confirm that the baby is growing appropriately and to give the mother and physician reassurance.
Lastly, bleeding can represent signs of a miscarriage or a pregnancy that has implanted in the wrong location (known as an ectopic pregnancy). Worrisome bleeding is bleeding that is heavy with passage of clots and/or accompanied by cramps and pain.
Most miscarriages occur due to a genetic abnormality within the embryo or fetus. If this is the case, then the miscarriage will be inevitable, and we will not be able to stop it. Ectopic pregnancies may also be accompanied by symptoms of abnormal bleeding and/or pain on one side. This problem if caught early can be treated medically, but it can also become a potentially life-threatening emergency.
If you are bleeding heavily—to the point where you are light-headed or soaking more than one pad per hour—you need to go to the emergency room.
I hope you come away from this post better informed about a few of the reasons you may experience bleeding during pregnancy—not all of which are related to a potential miscarriage. Again, whenever you experience vaginal bleeding, you should contact your physician immediately and follow their instructions!
It is always better to be safe than sorry, and it’s perfectly reasonable to feel anxious about your pregnancy—especially one that follows after miscarriage or loss. We are here to help.

Entire Website © 2003 - 2020
Karande and Associates d/b/a InVia
Fertility Specialists
