We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
In a recent issue of Contemporary Ob/Gyn, Drs Forman and Scott from Reproductive Medicine Associates of New Jersey published a summary of their work with the transfer of single embryos that had been screened for chromosomal abnormalities. Their results are excellent and here is a brief summary of what they have presented in the paper.
The majority of patients coming through IVF, especially after several failed IVF attempts, are reluctant to consider a single embryo transfer (SET). For them, twins, or even triplets, seem like a blessing. However, the medical community is all too aware of the complications of twin or triplet pregnancies. Preterm labor and delivery, arguably the most common complication, is currently costing the healthcare system an estimated $1 billion dollars a year. While triplet pregnancies have been on the decline, twin pregnancies after IVF remain steadily high. Intuitively, as a community of reproductive scientists and physicians, we know that singleton pregnancies are safer and have a lower risk of complications for our patients, and that is our end goal. The question is, however, how can we maximize our patients chance of a successful pregnancy while at the same time reducing the number of embryos transferred?
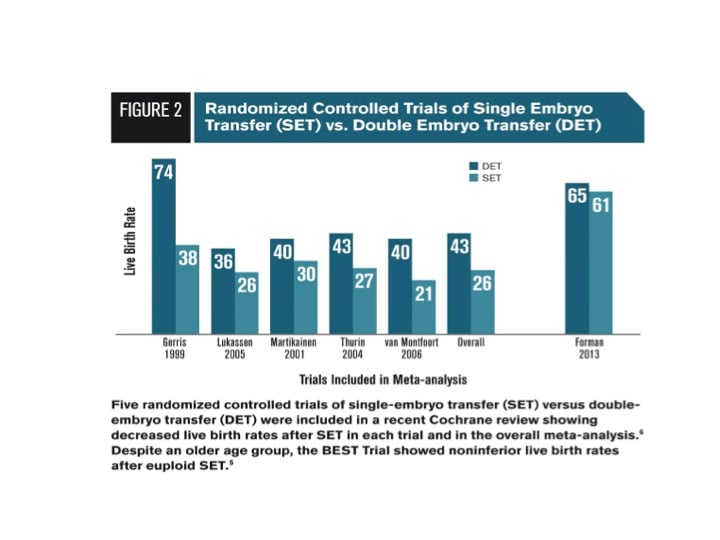
Many studies have been conducted showing the success rates following SET and double embryo transfer (DET). A recent meta-analysis in the Cochrane review compared five different randomized, clinical trials comparing SET and DET live birth rates and found that in all of the studies, the SET group showed a lower live birth rate than did their DET counterpart. With that amount of information showing statistically significant decreases in live birth rates following SET, is it possible to improve SET rates so as to maximize a patient’s likelihood of success while decreasing the number of cycles it takes to achieve a pregnancy?
Dr. Eric J. Forman and Dr. Richard Scott, both highly regarded reproductive endocrinologists, believe that there is a way to improve the success rates of SET; identify the embryo most likely to implant.
For the majority of patients, embryo selection is done by morphology alone. The embryo, or embryos, with the highest graded morphology get transferred. While this is not a bad way to perform embryo selection, it does not give us any information about the inner workings of the embryo, i.e. the chromosomal status. Using Preimplantation Genetic Screening (PGS), a test where some of the trophectoderm cells from the embryo are sent for analysis in order to determine the genetic karyotype of the embryo, the chromosomal status of the embryo can be known. Since we know that chromosomal errors are one of the main reasons that normal appearing embryos do not result in a live birth, logic follows that if we can transfer an embryo we know is chromosomally normal, wouldn’t that embryo have a higher chance of implanting and resulting in a baby?
In a word, yes.
The Blastocyst Euploid Selective Transfer (BEST) trial, conducted by Dr. Forman and Dr. Scott, was the first randomized trial to demonstrate that SET could be performed without the decrease in live birth rates that have been commonly seen. The BEST trial sought to compare PGS screened (euploid) SET against non-PGS screened DET. The results showed that the transfer a single euploid embryo had live birth rates that were comparable to the standard transfer of two embryos.
This is a very interesting finding, as it suggests that grading on embryo morphology alone is not enough to pick the embryo most likely to implant or to ‘be normal’. Of the 521 blastocysts tested in this study, 31% were abnormal, ranging from 21% in the younger patients and up to 56% in patients 40 and over. In women over 35, the occurrence of a blastocyst with good morphology to be aneuploid was found to be 40%.
It would seem that this study represents the direction the field of assisted reproductive technologies is headed, however, there are some limitations. Patients need to understand that insurance, as yet, does not cover the PGS cost, nor does insurance cover the cost to freeze the blastocysts (the blastocysts must be frozen while awaiting PGS test results). As the medical community is seeing the benefits of SET, hopefully one day that will change and insurance will begin to cover the cost. Until then, patients should begin to consider what transferring only one chromosomally normal embryo, thereby reducing the risk of the complications associated with multiple births, is worth to them.
To see a qualified fertility specialist with in-depth knowledge of PGS and SET, make an appointment at one of InVia Fertility's four Chicago area fertility clinics.

Entire Website © 2003 - 2020
Karande and Associates d/b/a InVia
Fertility Specialists
