We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
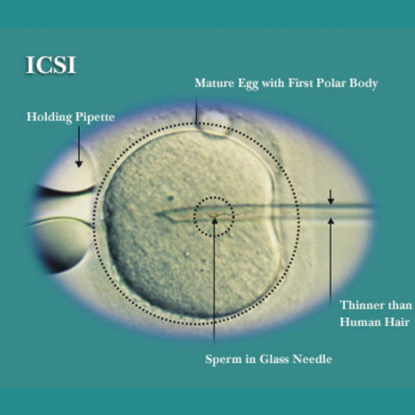
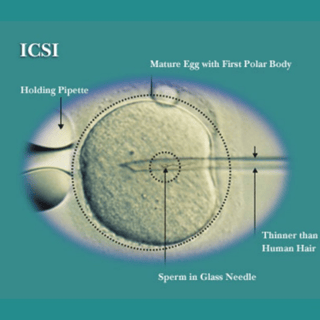 ICSI is an acronym for intra-cytoplasmic sperm injection. In basic terms it means we are injecting a sperm into an egg. ICSI IVF differs from the conventional IVF process in that a single sperm is injected into an egg, instead of fertilization taking place in a dish where millions of sperm are placed near an egg.
ICSI is an acronym for intra-cytoplasmic sperm injection. In basic terms it means we are injecting a sperm into an egg. ICSI IVF differs from the conventional IVF process in that a single sperm is injected into an egg, instead of fertilization taking place in a dish where millions of sperm are placed near an egg.
ICSI is usually applied when there is a male infertility problem such as defective sperm function. Male infertility can genetic in origin or result from environmental factors. Below is a list of common causes why ICSI is applied.
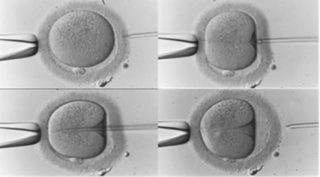 Overall, ICSI IVF is performed using specialized micromanipulation tools and equipment, along with the guided help of an inverted microscope to allow embryologist select, immobilize, and pick up an individual sperm into a carefully designed ICSI needle. Allowing them to carefully penetrate through the outer shell of the egg and inject the sperm into the cytoplasm of the egg.
Overall, ICSI IVF is performed using specialized micromanipulation tools and equipment, along with the guided help of an inverted microscope to allow embryologist select, immobilize, and pick up an individual sperm into a carefully designed ICSI needle. Allowing them to carefully penetrate through the outer shell of the egg and inject the sperm into the cytoplasm of the egg.
Some say there is an increased risk of birth defects with the use of IVF, specifically ICSI. However, studies have contradicted this theory. The Practice Committee of the American Society for Reproductive Medicine and the Practice Committee of the Society for Assisted Reproductive Technology considers ICSI a safe and effective therapy for male factor infertility. They also state that certain conditions may carry an increased risk for transmission of genetic abnormalities to the offspring, but do not know if it relates to the procedure itself, or to the characteristics of the couple who require ICSI.
When specific genetic abnormalities (e.g., abnormal karyotypes, Y chromosome microdeletions, CF mutations) are identified, affected couples should receive appropriate genetic counseling before proceeding with treatment. Only those fully apprised of risk for transmitting a genetic defect and its potential effect on their offspring should be offered ICSI.
To see a fertility specialist who is a board-certified physician with experience treating male and female factor infertility, make an appointment at one of InVia’s four Chicago area fertility clinics.

Entire Website © 2003 - 2020
Karande and Associates d/b/a InVia
Fertility Specialists
