We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.

 Embryo transfer is arguably the most critical step in the IVF process. On the surface, it seems like a relatively simple procedure. The embryos are loaded in a catheter and the physician deposits them through the cervical canal into the uterine cavity. It takes only a few minutes and is usually done with the patient wide awake, often with the partner right next to her.
Embryo transfer is arguably the most critical step in the IVF process. On the surface, it seems like a relatively simple procedure. The embryos are loaded in a catheter and the physician deposits them through the cervical canal into the uterine cavity. It takes only a few minutes and is usually done with the patient wide awake, often with the partner right next to her.
While it may seem simple, the devil is in the details. The embryos have to be gently (atraumatically) deposited in the uterine cavity in a location for optimal implantation or else the cycle will not work.
A recent publication by William B. Schoolcraft at the Colorado Center for Reproductive Medicine stressed the importance of embryo transfer technique in maximizing assisted reproductive outcomes. Here are some of the details.
Variables influencing IVF embryo transfer include performance of a trial transfer, contamination of the catheter tip with blood, mucus, or tissue from the uterine lining (indicating a traumatic transfer), as well as the occurrence of retained or expelled embryos. Other variable that influence outcome include the type of catheter used, the volume and type of transfer media, the presence of bacteria in the cervix or on the catheter tip, and the use of ultrasound guidance.
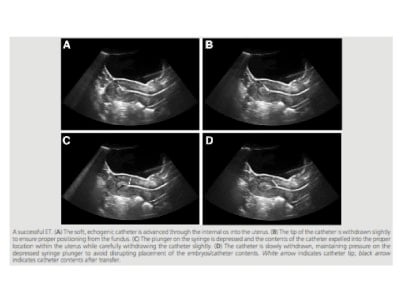 The goal is to avoid difficult embryo transfers. Here are some of the steps used to optimize clinical outcomes.
The goal is to avoid difficult embryo transfers. Here are some of the steps used to optimize clinical outcomes.
There are two types of catheters available: soft and stiff. It has now been conclusively shown that soft catheters have higher success rates when compared to stiff catheters. Soft catheters are believed to follow the contour of the uterine cavity more easily and thereby result in less risk of plugging the tip with blood, mucus or the uterine lining causing less “trauma” or disruption of the lining. A stylette or a stiff catheter can be used to get through the cervical canal. It is important that the tip not be advanced beyond the cervical canal (internal os). The obturator is then removed and the embryos that are loaded in a soft catheter (noodle) are passed through the central channel of the stylette into the uterine cavity.
Best rest is an absolute no-no. Many studies have shown no improvement in outcomes with bed rest. In fact some papers have shown lower pregnancy rates with bed rest.
IVF outcomes are decreased if there is a delay in transfer of embryos into the uterus after they have been loaded in the embryo transfer catheter. A delay of more than 120 seconds is believed to be significant. This is because the embryos are exposed to temperature changes and room air after they have been taken out of the controlled environment in the incubator. It could also be due to the fact that is delay is usually because access to the uterine cavity was difficult.
We will sometimes give patients Valium to help them relax. An occasional patient will require anesthesia for embryo transfer. We avoid dilating the cervix at the time of embryo transfer. Sometimes a stitch is placed in the cervix with the strings left long. This can be used to straighten out the cervix without causing uterine contractions. The use of hyaluronan (embryo glue) did not increase success rates when we used it at InVia.
To see a board-certified physician who is well versed in embryo transfer and has excellent success rates, make an appointment at one of InVia's four Chicago area fertility clinics.

Entire Website © 2003 - 2020
Karande and Associates d/b/a InVia
Fertility Specialists
