We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
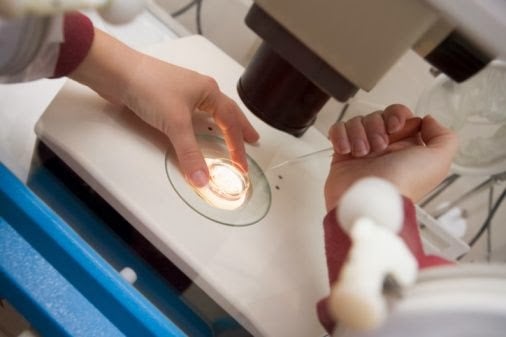
 In vitro fertilization (IVF) is now a fairly commonly used procedure and has resulted in the birth of tens of thousands of babies every year. According to the latest statistics available (2015, www.sart.org) there were 209,336 IVF cycles performed in the U.S. alone. This is an increase from 154,412 IVF cycles being performed in 2011.
In vitro fertilization (IVF) is now a fairly commonly used procedure and has resulted in the birth of tens of thousands of babies every year. According to the latest statistics available (2015, www.sart.org) there were 209,336 IVF cycles performed in the U.S. alone. This is an increase from 154,412 IVF cycles being performed in 2011.
In addition, the success rates with IVF have been steadily increasing with fewer embryos being transferred (details once again at www.sart.org). Initially, IVF was devised as a treatment for patients with diseased fallopian tubes (tubal factor). There have since been several other indications for IVF and a couple of brand new ones, which will be discussed in this blog.
For IVF to be successful it typically requires a healthy egg, sperm that can fertilize, and a uterus that can carry a pregnancy. But, what can be done in patients where this is not the case? This is where newer techniques such as preimplantation genetic diagnosis (PGD) to rule out presence of genetic disorders, as well as egg donation or surrogacy (where the woman providing the egg isn’t the same who will carry the pregnancy to term) can be used. Read on.
It is now possible to screen embryos for genetic or chromosomal abnormalities prior to transfer. PGD is indicated in:
There will be a series of blogs discussing these issues in further detail in the immediate future.
Egg freezing or embryo freezing can be offered to patients with cancer that may require surgery, chemotherapy or radiotherapy. In these cases, the cancer treatment can have a adverse impact on their fertility. By preserving eggs (or embryos), patients can potentially preserve their fertility and pursue pregnancy when ready.
In egg donation or embryo donation, the resultant embryo is transferred in another woman than the one providing the eggs. This is an excellent option for women with no eggs due to surgery, chemotherapy, or genetic causes; or with poor egg quality, previously unsuccessful IVF cycles or advanced maternal age.
In women who are not able to carry a baby, gestational surrogacy is an option. Women without a uterus (hysterectomy) or with uterine factors (multiple fibroids, abnormal uterine cavity (severe adhesions) or who are not able to carry a baby for other medical conditions are candidates for surrogacy. This is also an excellent option for gay couples (male) who wish to have a child.
Illinois is one of the few states with specific laws that make it possible for couples to use a surrogate to deliver the baby but have the genetic parents' name(s) on the birth certificate.
As you can see, it is now very common for couples to use IVF to have a baby. The pregnancy rates have been improving steadily. The procedure itself is getting to be less complex and has brought hope to thousands of couples who would otherwise be infertile.
Egg donation Infertility Infertility treatment IVF Male factor Embryo donation Egg freezing fertility preservation

Entire Website © 2003 - 2020
Karande and Associates d/b/a InVia
Fertility Specialists
