We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
-1.jpg)
-1.jpg?width=300&name=My%20Post%20(20)-1.jpg) Once a healthy, developing embryo is successfully transferred into your uterus, it has to attach itself to the uterine lining and then grow there, a process known as implantation.
Once a healthy, developing embryo is successfully transferred into your uterus, it has to attach itself to the uterine lining and then grow there, a process known as implantation.
For successful implantation, your uterine cavity must be "receptive". That means not compromised by inflammation, growths, or other problems, so that the embryo can "stick" and begin to grow.
In the fertility community, when we say "think sticky thoughts" after an IVF embryo transfer, this is what we're talking about. Lack of implantation or compromised implantation can lead to early miscarriage.
So, what kinds of issues can impact implantation, and how can your fertility team spot them?
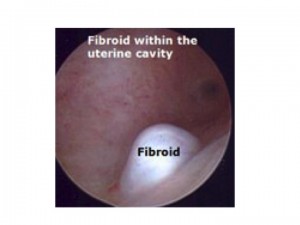
Uterine fibroids are benign tumors of the uterine muscle tissue. They are typically found in 5-10% of infertile women. Fibroids can affect the blood flow to an area of the uterus where they embryo may implant.
Depending on where the fibroid is, it may also cause irritation to the inside lining of the uterus which would also prevent implantation.
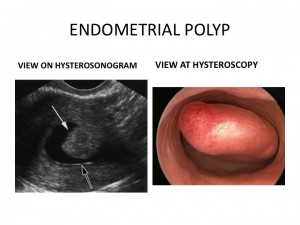 Endometrial polyps are an overgrowth of endometrial tissue that protrudes into the uterus. They are similar to ‘skin tags’ but inside the uterus. Polyps act like a naturally-occurring IUD, causing irritation and reducing the surface area available for an embryo to implant.
Endometrial polyps are an overgrowth of endometrial tissue that protrudes into the uterus. They are similar to ‘skin tags’ but inside the uterus. Polyps act like a naturally-occurring IUD, causing irritation and reducing the surface area available for an embryo to implant.
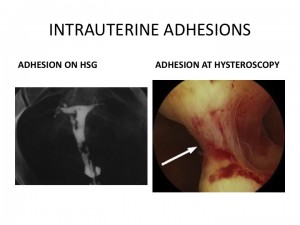
Uterine adhesions (scar tissue) may develop from previous uterine surgery or invasive procedures. This scar tissue can also form from endometrial infection. Severe scarring of the uterus is also referred to as Asherman’s syndrome.
This scar tissue blocks areas of the uterine lining where implantation may normally occur. It can also cause areas of minimal to no blood flow, which cuts your embryo off from nutrients.
Another uterine defect that may decrease implantation success is endometriosis. Endometriosis is found in 30-50% of infertile women. Endometriosis may cause adhesions, and it is also thought that endometriosis alters the environment of the uterus, making it less likely for an embryo to implant.
One example of an alteration affecting implantation is inflammation (swelling) of the uterine lining. This is not a conducive environment for an embryo to implant and continue to receive the nutrients it needs to divide properly.
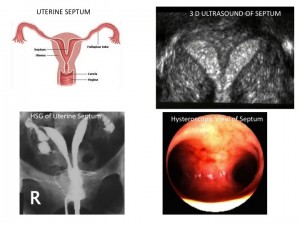
The final uterine factor affecting embryo implantation is the presence of a uterine septum. This is when the uterine fundus (top) extends down into the uterine cavity. This septum may extend all the way down into the cervix and only partially into the uterus.
Although it would seem this still leaves enough surface area for an embryo to implant, there is an inadequate blood flow to the septum. It has also been shown that the progesterone receptors on the septum may prevent implantation or cause problems if an embryo does manage to implant.
So how do you know if you have something inside the uterus preventing implantation? One test done frequently in the office is a HSG (hysterosalpingogram). This is an x-ray of the uterus. This test is performed by the physician. He/She will inject dye into the uterus while taking x-ray pictures. While this test tells us if your fallopian tubes are open or not, it can also detect many of the uterine abnormalities listed above.
Another common diagnostic test is an HSN (saline ultrasound). This is a vaginal ultrasound done by the physician. While performing the ultrasound, he/she will inject saline (water) into the uterine cavity. This test is helpful in detecting many uterine abnormalities also.
Finally, a patient may choose to have an HSC (hysteroscopy) done. This is a surgical procedure performed in the office which involves inserting a camera into the uterus to see what other imaging techniques may miss. Hysteroscopy is convenient for patients because in addition to being able to confirm diagnosis of an issue, the doctor can remove whatever may be present on the uterine lining preventing implantation.
Some, more serious uterine abnormalities, such as a severe uterine septum or invasive fibroids, may require a laparoscopy. This surgical procedure is done at the hospital and involves making small abdominal incisions to insert a camera and instruments to remove the abnormality.
In conclusion, embryos will have a better chance of implanting in uterine lining that is healthy and free of abnormalities that may be decreasing the amount of surface area available. There are many diagnostic tools in place to detect these uterine defects early enough so that treatment can take place, further increasing your chance at achieving a successful pregnancy.
Infertility Infertility treatment IVF InVia Fertility Specialists

Entire Website © 2003 - 2020
Karande and Associates d/b/a InVia
Fertility Specialists
