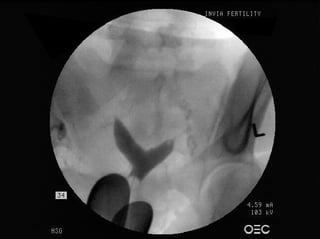
 A uterine septum is a common anomoly of the uterus that is seen in 1 – 15 per 1,000 women (shown in the picture at right). In this condition, the cavity of the uterus is separated by a long piece of tissue, while the outside of the uterus has a normal shape.
A uterine septum is a common anomoly of the uterus that is seen in 1 – 15 per 1,000 women (shown in the picture at right). In this condition, the cavity of the uterus is separated by a long piece of tissue, while the outside of the uterus has a normal shape.
According to several studies, treating a uterine septum is associated with an improvement in live-birth rates for women with prior pregnancy loss, recurrent pregnancy loss, multiple miscarriages, or infertility.
In a uterine septum, a wall or wedge of tissue divides the uterus; it is composed of muscle fibers and some connective tissue. It may be complete, dividing the uterus into completely separate chambers, or partial. The size and shape of the septum can vary by width, length, and blood supply.
A complete septate uterus has a single uterine fundus, with a septum extending from the top of the uterine cavity and continuing through the cervix. A partial (incomplete) septum refers to a single fundus and cervix with a uterine septum extending from the top of the uterine cavity toward the cervix.
The indentation of the uterine musculature should be more than 1.5 cm for it to be called a septum. When the indentation is less than 1 cm it is called normal or arcuate (an arcuate uterus is not clinically relevant).
The Practice Committee of the American Society for Reproductive Medicine recently published guidelines for the diagnosis and treatment of a uterine septum. Here are the answers to 10 frequently asked questions about uterine septum:
- How is a uterine septum diagnosed? The gold standard method requires direct visualization of the exterior and interior of the uterus using laparoscopy and hysteroscopy. These are relatively invasive and currently, imaging techniques are the preferred modality to diagnose uterine septum. Use of X-ray (hysterosalpingography) is often the initial test to diagnose an anomaly. However, it is not possible to differentiate between a septate uterus and a bicornuate uterus (double uterus) with X-ray. Use of ultrasound (hysterosonogram or sonohysterogram) is a good technique for diagnosing a uterine septum. Saline is injected in the uterine cavity with concurrent vaginal ultrasound scanning. This enables one to visualize the inner as well as the outer contour of the uterus. 3-dimensional (3-D) ultrasound combined with saline infusion has 100% accuracy when compared with surgery. Magnetic Resonance Imaging (MRI) can also be used for diagnosis; however, it is a very expensive test.
- Does uterine septum cause infertility? No, it does not. However, there are studies that show a higher pregnancy rate in women who have hysteroscopic uterine septum removal (resection).
- Does a septum contribute to miscarriages or adverse pregnancy outcome? There is fair evidence that uterine septum contributes to miscarriage and preterm birth. A uterine septum may increase the risk of other adverse pregnancy outcomes such as the baby being bottom down (breech) or tranverse, intrauterine growth restriction, placental separation and bleeding (abruption) and perinatal mortality.
- Does treating a septum improve obstetrical outcomes? Yes. There, however, is limited information available on this issue. Some studies do show that hysteroscopic septum incision reduces miscarriage rate and improves live-birth rates in patients with a history of recurrent pregnancy loss and infertility.
- Does size or shape of the septum correlate with reproductive outcome? No it does not. Review of patient records with partial vs. complete septum and small vs. large septum have showed similar incidence of miscarriage and late pregnancy complications.
- What is the best surgical technique for incising a uterine septum? Historically, it a large abdominal incision (laparotomy) was used to operate on a uterine septum. This has now been replaced by hysteroscopy. Operative hysteroscopy can be performed in the office or in the hospital. Commonly used techniques include incision of septum utilizing cold scissors, electrical current (unipolar or bipolar cautery) or laser. The outcomes with the different hysteroscopic techniques are similar. The choice should be based on the surgeon’s preference. Some surgeons will use laparoscopy and others use ultrasound to help with the surgery. At InVia, we have a great deal of experience with this kind of surgery, and we do office-based hysteroscopic surgery of uterine septum.
- How long after surgical treatment of a uterine septum should a woman wait to conceive? There is no specific time that is recommended. Since the uterine cavity is healed two months post-operatively, that should be a sufficient waiting time. However, there have been studies where pregnancy was achieved within a month of treatment with excellent outcomes.
- Is it necessary to use medications to thin the uterine lining prior to surgery? Medications used for this purpose include Danazol and Lupron (a gonadotropin releasing hormone agonist). Studies have shown that these do not improve outcomes and do not reduce scar tissue (adhesion) formation.
- After surgery, is adhesion prevention needed? The techniques used include use of hormones (estrogen), mechanical devices including balloon catheters, and intrauterine devices. The incidence of scar tissue formation after septum surgery is very low and use of these adjuvants do not improve outcome.
- What are the complications after hysteroscopic surgery for uterine septum? There have been 18 case reports in the literature of uterine rupture during pregnancy or delivery following septum incision. The risk of this happening is increased with excessive septal excision, penetration of the uterine musculature (myometrium), making a hole in the uterine wall, and excessive use of cautery or laser energy during the septum incision procedure.
To see a fertility specialist with in-depth experience providing office-based hysteroscopic surgery to treat uterine septum, make an appointment at one of InVia’s four Chicago area fertility clinics.
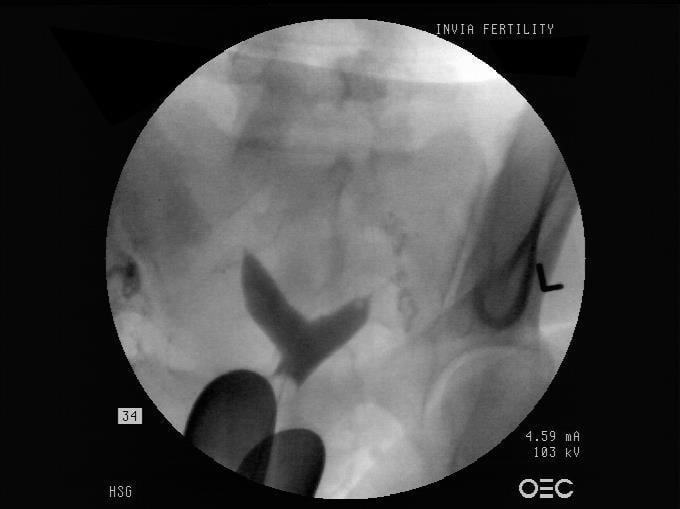
 A uterine septum is a common anomoly of the uterus that is seen in 1 – 15 per 1,000 women (shown in the picture at right). In this condition, the cavity of the uterus is separated by a long piece of tissue, while the outside of the uterus has a normal shape.
A uterine septum is a common anomoly of the uterus that is seen in 1 – 15 per 1,000 women (shown in the picture at right). In this condition, the cavity of the uterus is separated by a long piece of tissue, while the outside of the uterus has a normal shape.
