We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
We are experiencing a very high volume of calls and messages and ask for your patience. We will answer your portal messages within 48 hours.
 We often talk about follicles (affectionately called "follies") during the IVF process. But IVF patients often don’t understand the difference between follicles and eggs. If eggs aren't follicles, what are follicles, anyway?
We often talk about follicles (affectionately called "follies") during the IVF process. But IVF patients often don’t understand the difference between follicles and eggs. If eggs aren't follicles, what are follicles, anyway?
The follicle is the anatomical structure in which a mature egg or oocyte is released. Doctors are sometimes responsible for the confusion between eggs and follicles, because we usually loosely refer to the follicles we see on your ultrasound scan as eggs. This is especially true during IUI cycles; or when a sonographer or technician is doing the scans. When she sees that your ovaries have responded well to the superovulation, she will often say, "Good, your eggs are growing well."
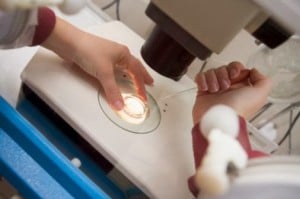
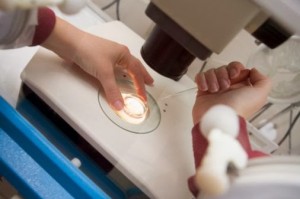
In reality, eggs are microscopic structures, which cannot be seen on ultrasound scans. They are only 100 microns (0.1 mm) in size, and can only be seen by the embryologist in the IVF lab when scanning the follicular fluid received from the doctor (gathered during egg retrieval) under the stereozoom microscope.
Ultrasound scans allow us to track the growth of the follicles in your ovaries. Follicles are seen as tiny black bubbles on the scan, because they contain follicular fluid. They range in size from 4 mm – 25 mm; and the eggs grow within these follicles. However, not all follicles contain eggs, which is why the correlation between the numbers of follicles seen on the IVF ultrasound scans and the number of eggs, which are actually retrieved is not perfect.
When all the follicles grow at the same rate (a synchronous cohort), then timing the hCG trigger is much easier. However, often the growth is asynchronous; and some follicles may become big while the others remain small. It can be very difficult for the doctor to time the hCG in such patients.
Thus, you may be disappointed when the doctor gets fewer eggs as compared to the number of follicles counted at the time of giving the hCG trigger. This is because some follicles are small and don't contain eggs; while others are large, and have formed cysts which do not have an egg. It’s not possible to differentiate between a cyst and a large follicle based on the ultrasound scan images. It’s only after the doctor sends the follicle fluid to the embryologist in the IVF lab will we know whether there is an egg in it or not.
Another possibility for not getting as many eggs as expected is that the doctor may have technical problems during egg retrieval, and may not be able to reach the follicle (for example, when the patient is obese and the procedure is being done without general anesthesia). Some doctors may not do a good job with aspirating each follicle, and may fail to collect the egg, because they do not flush the follicle completely and the egg remains stuck to the follicular wall; or because there is too much blood; or because the embryologist may not be experienced at identifying the egg.
This is especially true when there are only a few eggs; or if the doctor is not experienced; or if there are too many cases scheduled on that day and the doctor is in a hurry to complete your procedure.
In the extremely rare case of empty follicle syndrome, there are no eggs present in the follicles when egg retrieval is attempted.
Sometimes, we may also get more eggs than the number of follicles counted on the scan. This is because doctors may not bother to diligently count all the follicles seen on the ultrasound scan; or that some follicles are hiding behind the others, which is why they may not be seen during the scan.
Even if the doctor does manage to retrieve all the eggs, do remember that not all the eggs will be mature; and that not all will fertilize.
Because we are interested in the quality and the quantity of the eggs, we also track the blood levels of estradiol during the IVF cycle. Estradiol is not produced by the egg, but by the granulosa cells which line the follicle. As the follicle matures, it increases in size and the number of granulosa cells also increases, as a result of which the estradiol levels rise progressively. Estradiol levels help us to determine when the follicles are mature, so we can time the hCG trigger properly, and maximize the number of mature eggs we retrieve.
While the correlation between estradiol levels and the number of mature eggs collected is quite good, it’s not always perfect. This is why IVF doctors need a lot of experience and expertise when interpreting these scans. This is especially true in older women; patients working on getting pregnant with PCOS; and those with poor ovarian reserve, as the margin for error in these patients is very thin.
To see a fertility specialist who is a board-certified physician with excellent success rates, make an appointment at one of InVia’s four Chicago area fertility clinics.
Infertility treatment IVF Embryology Understanding Test Results

Entire Website © 2003 - 2020
Karande and Associates d/b/a InVia
Fertility Specialists
